Why do my toes and fingertips change colors? |
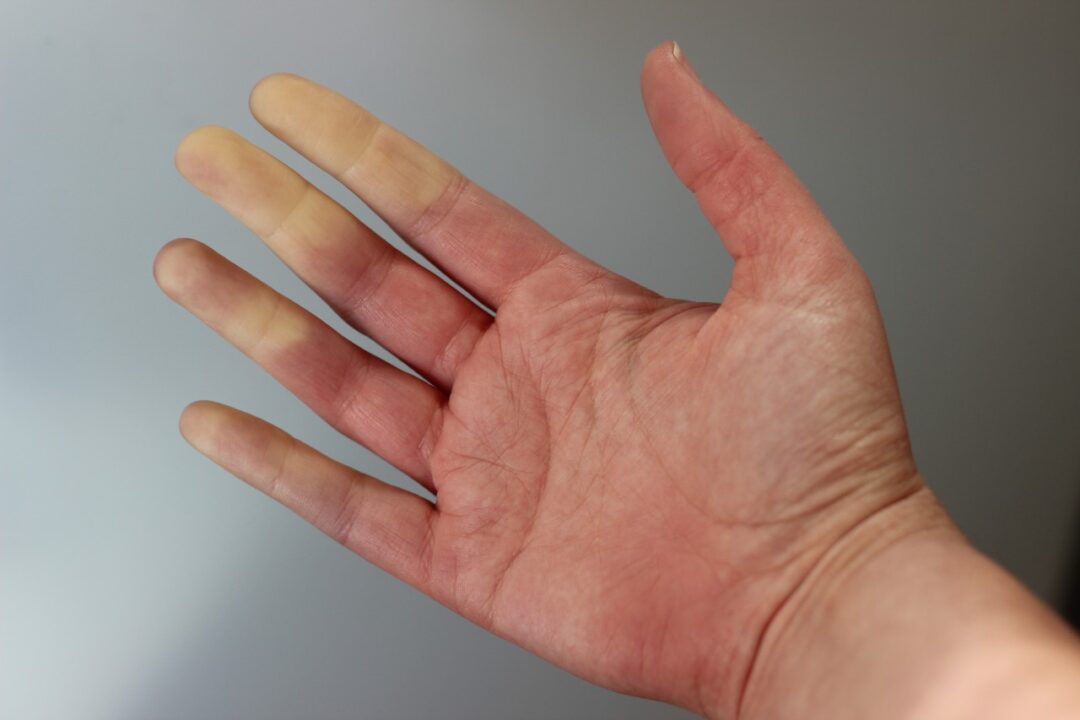
Raynaud’s (ray-NODES) is a condition that affects blood vessels, primarily in the fingers and toes. It was named for Dr. Maurice Raynaud, a French physician who first described the condition in a young woman whose fingertips changed colors when she was cold or under stress. There are two primary types of Raynaud’s. The first, known as Raynaud’s Disease or Primary Raynaud’s, is a relatively benign condition with no known underlying cause. The second, referred to as Raynaud’s Syndrome or Secondary Raynaud’s develops in conjunction with an underlying medical condition.
What happens during an episode? The manifestations of Primary Raynaud’s usually develop as an exaggerated response to cold. While it is normal for blood vessels in the skin to constrict in order to maintain core temperature, in Raynaud’s the blood vessels narrow to the point that blood flow is markedly restricted. This is usually noted in the fingers or toes, often with the classic color changes—white, blue, and red. First, the digits turn white as a result of restriction of blood flow. This may be followed by numbness, tingling, and a bluish discoloration of the skin. Once the circulation begins to return the affected digits turn red and throb prior to returning back to normal. Symptoms last until the skin is rewarmed, after which normal blood flow to the skin recovers in around 15 minutes.
Who gets Raynaud’s? Raynaud’s is thought to affect up to 10% of the population, with the great majority of these having Primary Raynaud’s. Primary Raynaud’s is more common in women than in men, usually developing before the age of 30. Although a definite genetic link for Primary Raynaud’s has not been established, in many families, more than one member has the condition. Secondary Raynaud’s usually begins after the age of 30 and often develops in conjunction with a connective tissue disease, such as scleroderma or lupus. It can also develop in people who have sustained injuries or frostbite to the hands and feet, smokers, and workers performing repetitive tasks or using vibrating tools.
How is Raynaud’s diagnosed? There is no single blood test available to diagnose Raynaud’s phenomenon. The characteristic color changes and precipitating factors often provide enough information for a doctor to make the diagnosis. Distinguishing the primary from the secondary form, however, may be more difficult. Questioning about possible secondary factors—injuries, occupational hazards, medications, etc.—may provide the underlying cause. In cases where connective tissue disease is suspected tests such as the antinuclear antibody (ANA) or erythrocyte sedimentation rate (ESR or “sed rate”) may be performed.
How is Raynaud’s treated? Primary Raynaud’s has no cure. Fortunately, symptoms are typically mild and not associated with any blood vessel or tissue damage. When treatment is necessary, the following lifestyle measures help in most cases:
- Take measures to avoid becoming cold in the first place. Wear a hat, mittens (rather than gloves), scarf, coat with snug cuffs, and warm socks and shoes during cold weather. Layer your clothing for extra warmth. If necessary, use commercial hand warmers or battery powered heated gloves.
- Warm the body and the hands or feet at the first sign of an attack. If outside in cold weather, go indoors. Run warm water over your fingers or toes or soak in a hot tub.
- When fingers are involved, swinging the arms in large circles helps to increase circulation.
- Avoid smoking. The nicotine in cigarettes causes blood vessels to narrow, which may lead to an attack.
- Avoid taking certain medications. Vasoconstrictors including beta-blockers (e.g. metoprolol, propranolol, others) and migraine headache medications in the triptan class (sumatriptan rizatriptan, zolmitriptan, eletriptan, others).can be responsible for triggering Raynaud’s.
- Control stress. If stress triggers attacks, try to remove yourself from the stressful environment. Relaxation techniques or biofeedback can also help decrease the number and severity of attacks.
Some people with Raynaud’s, particularly those with a secondary cause, can develop serious complications, such as ulcerations on fingers or toes. In addition to lifestyle measures, these individuals may require treatment with medications. When medications are required, those that dilate blood vessels, such as calcium channel blockers (nifedipine, amlodipine, others) are considered to be the first line treatment. Another class of high blood pressure medications, alpha receptor blockers prazosin (Minipres) or doxazosin (Cardura) help in some cases.
What’s on the horizon? Research is being conducted into more effective diagnostic measures, such as the use of laser contrast imaging, as well as new treatments to improve blood flow for those who have Raynaud’s.
If you have any more questions just Ask Hanna, our health advisors are here to help.
Image: ©Shutterstock / Amanda Uhlin